Manufacturer Focusing On Medical And Surgical Laser Systems
Dimed Lasers has consistently delivered the most innovative technologies in medical laser market.
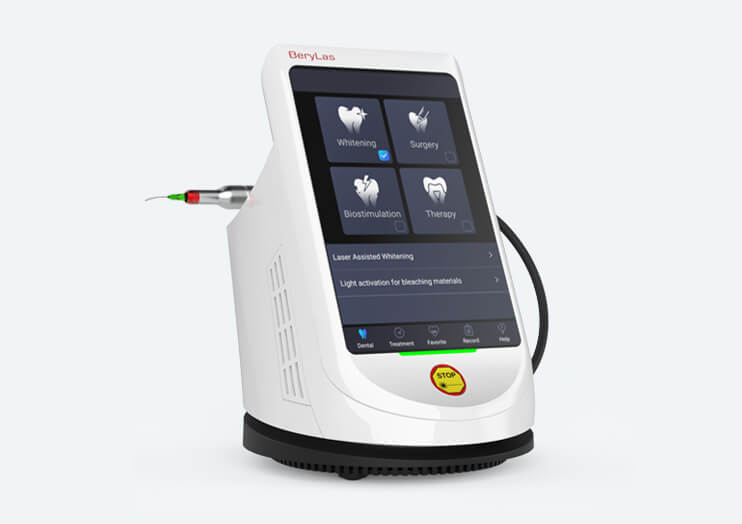
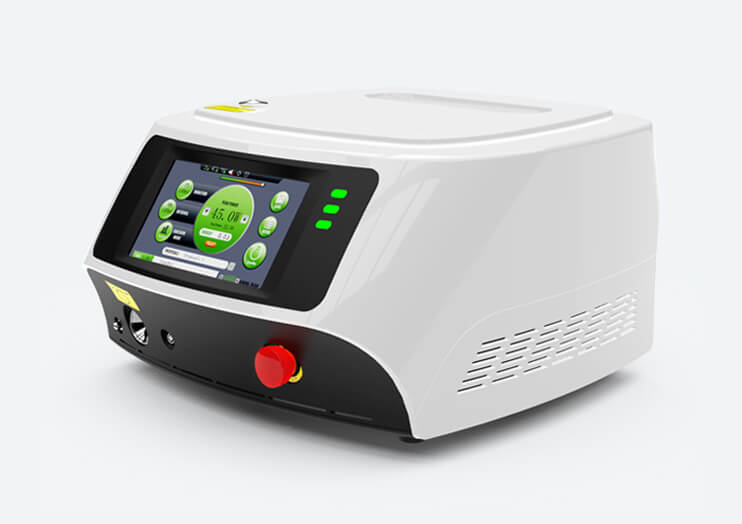
The undisputed classic mini diode system 30watts (15watts+15watts) with dual /three
wavelength technology
Laser Treatments
Dentistry, PLDD, high-intensity laser therapy, spider vein removal,
nail fungus treatment, veterinary endovenous laser treatment, hemorrhoids…
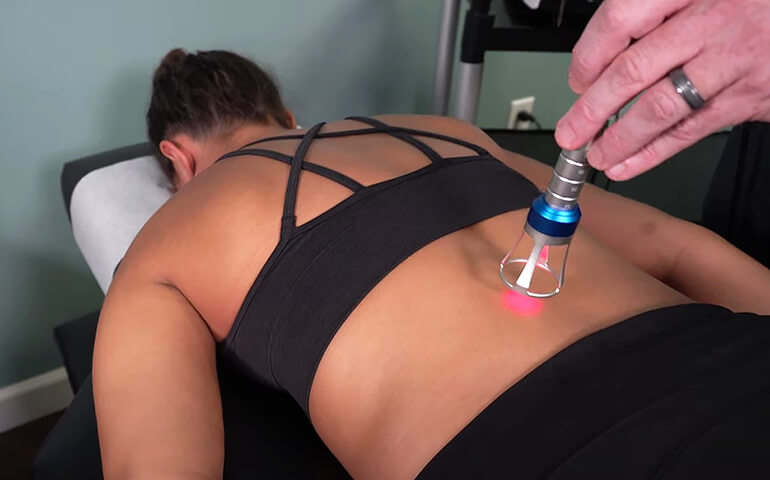
Class IV Laser Therapy
High Power Class 4 Laser Therapy In Physiotherapy Laser therapy light is infrared electromagnetic energy entering the body as ...
Veterinary
Pet Therapy Laser For Your Best Veterinary Experience Surgery and General Surgery Surgical lasers have become a very important ...
Endovenous Laser Treatment
What Is Endovenous Laser Treatment (EVLT Laser)? Endovenous Laser Ablation Treatment, also known as endovenous laser therapy, is a ...
Hemorrhoid Treatment Laser
Hemorrhoids (also known as "piles") are dilated or bulging veins of the rectum and anus, caused by increased pressure ...
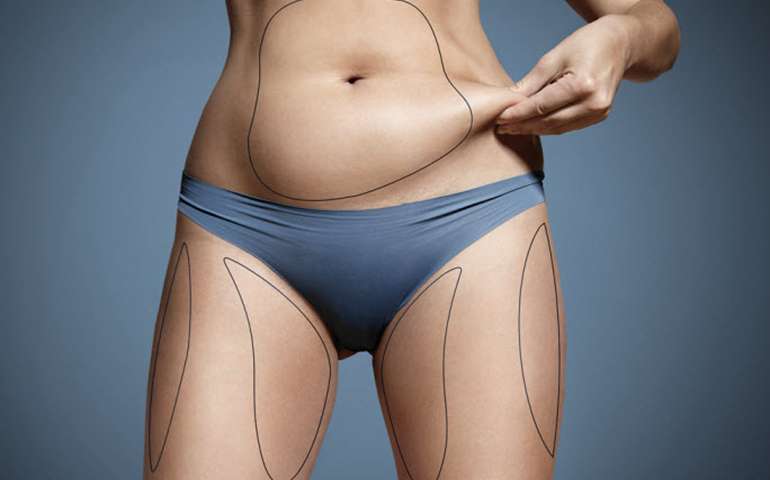
Laser Lipolysis
Laser-assisted lipolysis is a minimally invasive procedure for the removal of stubborn pockets of fat. It can effectively ...
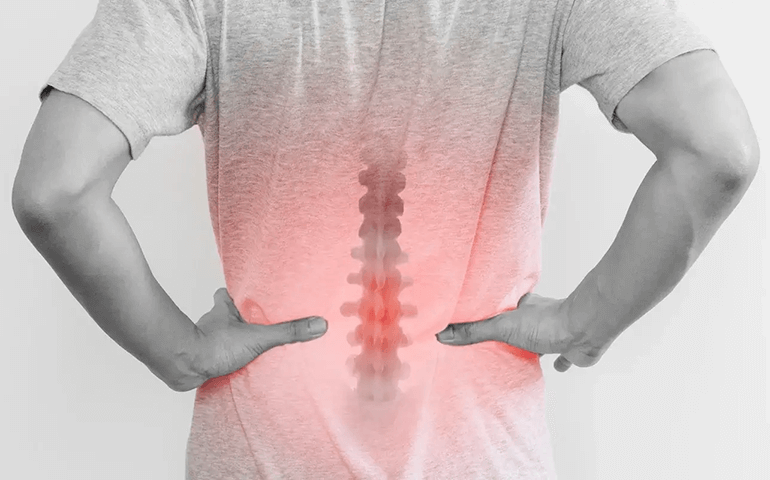
PLDD Laser
The Principle Of PLDD In the procedure of percutaneous laser disc decompression, laser energy is transmitted through a thin ...
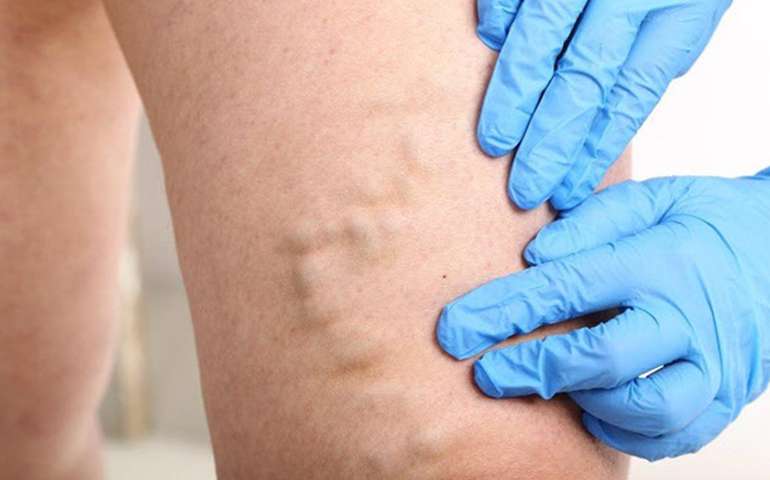
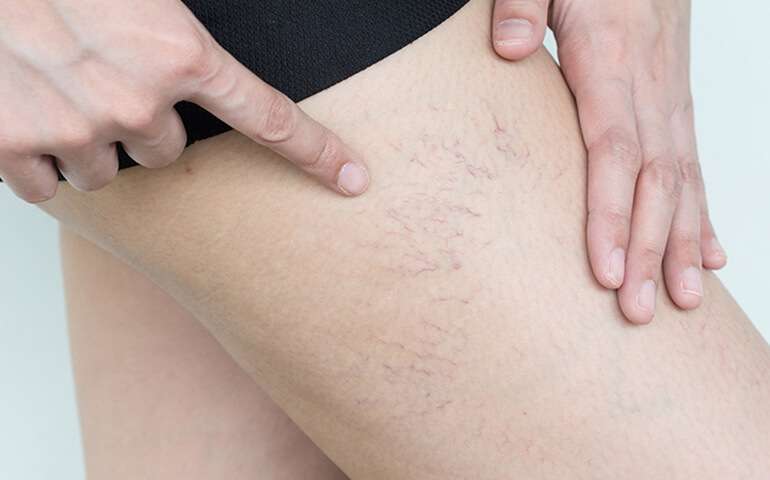
Laser Spider Vein Removal
Telangiectasias, commonly known as Spider veins, are usually tiny dilated blood vessels beneath the skin surface and calibrated between ...
Gynecology Laser Treatment
Cosmetic Gynecology As the age of a female grows, the vagina may lose collagen or tightness, which is known ...
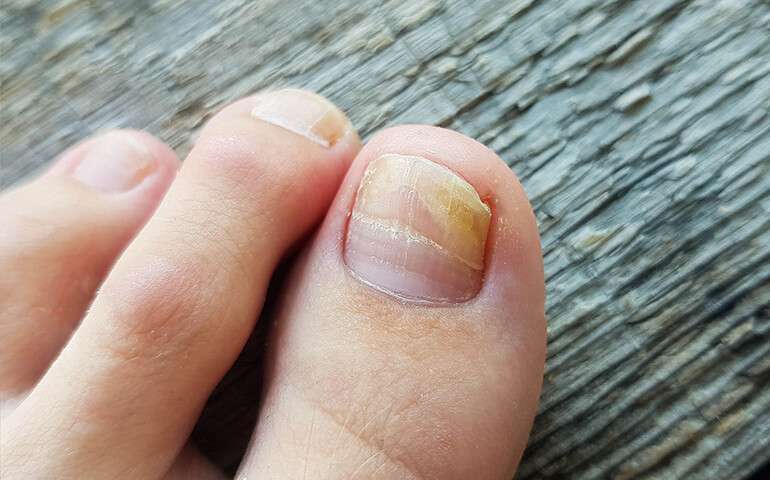
Laser Nail Fungus Treatment
Fungal nail disease, medically referred to as onychomycosis, affects many people. Fungi that feed on keratin, a structural protein ...
Latest News
Dimed Laser news, health and medical articles, such as medical treatment technologies,
laser therapy techniques, exercise tips, health maintaining knowledge and etc.
2024 Spring Team Bonding Day at Dimed Laser
2024 Spring Team Bonding: A Day to Remember! As the cherry blossoms began to bloom and the crisp air of spring whispered promises of renewal, the Dimed Laser team gathered on ...
Join Dimed Laser at FIME 2024 in Miami, USA
We are thrilled to announce that Dimed Laser will be exhibiting at the Florida International Medical Expo (FIME) 2024, and we invite you to visit our booth for an exclusive look at our innovative medical laser solutions. See you at FIME 2024!
Thank You for Visiting Dimed Laser at AEEDC Dubai 2024
Dimed Laser was delighted to join the AEEDC Dubai 2024 Exhibition, the world's largest annual scientific dental conference and exhibition, from February 6 to 8, 2024, at the Dubai World Trade Centre. Thank you for your visit and see you next year!